
Practice Perfect 861
Radiculopathy: The Most Hated (and Missed?) Podiatric Diagnosis Part 1
Radiculopathy: The Most Hated (and Missed?) Podiatric Diagnosis Part 1
As podiatrists, we see a lot of patients with heel pain. A lot! The majority of the time, the diagnosis is “simple” plantar fasciitis. But sometimes it’s something else. Neurological problems such as Baxter’s neuritis, medial calcaneal neuritis, and tarsal tunnel are local and well within the purview of podiatric care. However, spinal radiculopathies may also cause heel pain, and, unfortunately, are not directly treatable by podiatrists. Personally, I find this diagnosis to be my least favorite (since I can’t do much to treat it), and it is also commonly missed by many doctors, podiatric physicians included. I’ve seen a large number of patients for second opinion for recalcitrant heel pain in which the diagnosis was originally plantar fasciitis but was actually radiculopathy. Let’s review this challenging diagnosis in two parts. Today we’ll examine the pertinent anatomy with an emphasis on the structures that may cause lumbosacral radiculopathy. Next week, we’ll apply this anatomy to a rational neurological examination.
Question: What is radiculopathy?
The word “radiculopathy” derives from the Greek “radix” (root) and “patheia” (suffering). The spinal root is compressed in some way as it exits the canal between two vertebral bodies. Anything that can compress these nerves as they run through or exit an area of the spine can create symptoms. Pain described as “radicular” is often shooting in quality.
Question: What important anatomy should we know?
The anatomy of the spine is highly complex, but it is necessary to have a solid understanding of the structures interacting with the spinal cord and the nerve roots when considering patient complaints. Referring to Figure 1, there are some specific structures we can focus on to explain the most common causes of compression1.
- Disc Herniation – This is the most common cause of radiculopathy, resulting from the nucleus pulposus of the intervertebral disk breaking through the annulus fibrosus, thereby pushing against the cauda equina.
- Thickened Ligamentum Flavum – This is the ligament lining the spinal canal, connecting the vertebra, and sitting just posterior to the spinal cord. If this thickens, it will narrow the spinal canal.
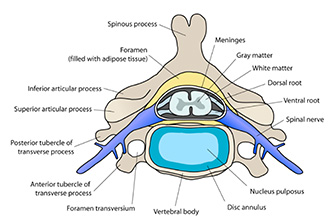
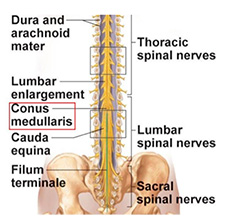
Figure 1. Coronal view of the spinal cord with emphasis on the area around the nerve roots (transverse vertebral view) and the cauda equina (coronal view)2.
- Spondylolysis and Spondylolisthesis – If the superior articular process fractures (spondylolysis) then the vertebral body may start to slide forward (spondylolisthesis) leading to nerve compression.
- Facet Hypertrophy – There is a facet sitting on top of the superior articular process of the vertebra that articulates with the vertebra above, but in degenerative arthritis, that facet may enlarge and compress the spinal nerve or the root.
It is important to note that all lumbar and sacral nerve roots begin at the T12 and L1 levels and then course downward to exit their respective intervertebral foramina at a different level from where they arose. Remember, then, that the L1 – S5 nerve roots do NOT come directly out of the spinal cord and then through the corresponding foramen but rather create the cauda equina (named after a horse’s tail because that’s exactly what it looks like!). As a result, damage to higher spinal levels may affect lower spinal roots, and compressing the cauda equina, with all of its freely hanging nerves, is compressible in a different way than the higher levels of the spinal cord. For example, this anatomy, with multiple nerve roots in one area, allows for simultaneous bilateral root compression which may lead to bilateral symptoms.
With this important anatomical understanding, and an appreciation for how radiculopathy occurs, next week we will explore components of the neurological examination to identify those patients with the disorder.
Best wishes.

Jarrod Shapiro, DPM
PRESENT Practice Perfect Editor
[email protected]

-
Hsu PS, Armon C, Levin K. Acute lumbosacral radiculopathy: Pathophysiology, clinical features, and diagnosis. UpToDate, Updated 8/27/21. Last accessed 4-22-23.
Follow this link -
Creative commons use. Cardimage_2842722_01335862646499.jpg. Last accessed 4-21-2023.
Follow this link
































Comments
There are 0 comments for this article