
Practice Perfect 844
Eminently Preventable
Eminently Preventable
I just got off call early this morning. It’s a Friday, the week after New Year’s. My call group covers local hospitals, and we each do one week at a time starting Friday mornings and ending the following Friday morning. I was the lucky soul this year to be on call during the change in years from 2022 to 2023. It was a bit challenging for me to be in the hospital seeing patients during New Years, but just imagine how difficult it was for the patients. Instead of being at home with family and friends, they were laying in the hospital with infections and complications, hooked up to IVs, being poked and prodded at all hours. What a lovely way to spend the holiday, huh?
And it was all eminently preventable.
Every podiatrist who sees patients in the hospital (a vast majority of us, I’ll wager) know exactly what I’m talking about: lower extremity complications from diabetes. During my call week, the on-call resident and I did two I&Ds, two partial 5th ray amputations, a transmetatarsal amputation, several wound debridements, and referred two patients for major limb amputations.
And they were all eminently preventable.
But they were not only preventable in the immediate past. The worst part is that the complications related to diabetes are preventable at multiple points in every patient’s life. Take a look at the figure below that shows one model in which a patient slides down the slippery slope from a diabetes diagnosis to a limb amputation.
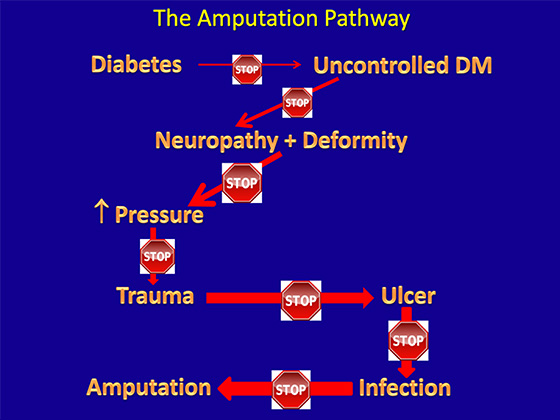
Note in the figure above a patient slides down the slippery slope from a diabetes diagnosis to a limb amputation.
The most notable aspect of this pathway from the diagnosis of diabetes to the loss of a limb is how many steps there are. A nontraumatic limb amputation in a diabetic may be a surprise to some patients, but they never are to those of us trying to prevent them. I can’t remember if I’ve ever looked at a foot infection and thought, “Wow that came out of the blue.” There was always something that precipitated the emergency situation.
Diabetic foot infections don’t “come out of the blue”. There was always something that precipitated the emergency situation.
Notice next that each step is entirely preventable. I count SEVEN unique steps, each with its own intervention, each avoidable. Notice also that the arrows become progressively thicker and larger as we proceed down the venous fly trap path toward amputation. This is no yellow brick road! This indicates that the further down the path we go, the more damaging to the patient things have become. We know that controlling blood sugar prevents neuropathy, which reduces the risk of everything else downstream. Similarly, once a patient sustains a neuropathic ulcer, the risk of limb and life-threatening complications is much greater – and so much more difficult to move back up the path toward more healthy conditions.
Note on the figure above that the further down the path we go, the more damaging to the patient things have become.
On a positive note, we are lucky to have interventions available at all stages of this pathway. Granted, we don’t want to intervene with some of our methods, such as amputations, but at least we have tools to heal wounds, improve blood flow, improve nutrition, lower blood sugar, and, in many cases, improve patients’ lives.
What do we do with this knowledge? Well, it seems obvious: prevent the entire chain of events. Stop diabetes from occurring in the first place. So much easier said than done! Since we don’t yet have a medical cure, the most effective prevention is maintenance of a healthy weight and physical activity. Let’s just eliminate the obesity epidemic. Good luck.
What can podiatric physicians do to help with this? Besides what we’re currently doing saving limbs with interventions such as wound care, surgical procedures to eliminate deformity, and, when necessary, targeted amputations that allow continued ambulation, we should continue educating our patients and providers about the need for all diabetics to receive foot screening and prevention interventions as well as there being someone to reach out to when a complication does happen. It’s much easier for us to intervene with debridement and offloading of a small wound at the start than having to amputate part of the foot a month later after a life-threatening but eminently preventable infection. Keep up the fight, and I’ll see you on the wards.
Best wishes.

Jarrod Shapiro, DPM
PRESENT Practice Perfect Editor
[email protected]

































Comments
There are 0 comments for this article