
Practice Perfect 827
Making Practice Perfect Decisions
Part 4 - Consider the Patient
Making Practice Perfect Decisions
Part 4 - Consider the Patient

Welcome back to our ongoing series about making Practice Perfect Decisions. In the first three parts, I presented a general framework to make treatment decisions by identifying the damaged anatomy, appreciating the underlying pathomechanics, and focusing treatment on those pathomechanical issues by adjusting forces and fixing deformities. Today, we will move on to more specific aspects with Rule #4:

This rule may be alternately named, “Welcome to the real world.” In school, we are taught the academic approach, as if the world is black and white. For example, students are still taught to base bunionectomy procedure choice on the size of the intermetatarsal angle. In reality, though, considering academics in isolation is only good for examination questions and often is not effective for actual patients. For example, some patients may not be able to undergo certain procedures for various reasons. Maybe they can’t be non-weightbearing or they’re too unhealthy for an open procedure. Sometimes the best choice is the one that best improves pain while allowing the fastest return to activity or lower healing risk.
- Age – Physiologic age is more important than chronologic age. I have taken care of 80-year-olds healthier than some 65-year-olds.
- Weight – Obesity is a major issue with many of our patients, and this will often be an important factor in determining the type of approach. For example, the foot orthosis shell needs to be thicker for these patients, but perhaps more significantly, obesity may necessitate joint fusion procedures rather than osteotomies.
- Situational needs – Obtaining a clear understanding of a patient’s personal life and situation is important to predict postoperative problems. A common challenge is someone with a right foot problem that requires surgery, but they must continue to drive. This problem might eliminate surgery as an option.
- Ability to rehab/weight bear – In my opinion, this issue has become somewhat less significant for many forefoot surgeries, as a solid base of research has demonstrated safe weightbearing after procedures such as the Lapidus bunionectomy and 1st MTP joint fusion, among others. However, hindfoot procedures such as fusions remain non-weightbearing postoperatively and may necessitate circular external fixation if the patient must bear weight. Is the patient strong enough to use crutches, walker, or knee scooter? Maybe they will need preoperative physical therapy to prevent postoperative complications.
- Comorbidities – Most medical conditions create relative contraindications for lower extremity surgery. For instance, diabetes is relatively contraindicated, but can be safely performed in patients with an A1c below 8% and adequate arterial flow. A less invasive approach may be necessary for those with less controllable diseases but who must still have surgery.
- Vitamin D/Bone healing ability – The more time goes by, the more I become aware of the prevalence of vitamin D insufficiency and this deficiency’s effects on bone healing. Even in sunny California this disorder is rampant.
- Tissue quality – Obviously, the worse the skin, the more likely there will be healing complications. Skin atrophy, pigmentation, and tension may require less invasive surgical approaches or avoidance of surgery altogether. Similarly, certain areas such as around the Achilles region are prone to dehiscence. These complications may be reduced through certain incisional approaches and considering the vascular anatomy.
- Anticipated shoewear – It is more important to understand the patient’s expectations rather than targeting a surgery for a specific type of shoe. A patient expecting to wear high heels after a bunionectomy procedure is a patient bound to be dissatisfied after surgery.
- Expectations – Could we have left the most important for last? Perhaps the most important part of any discussion whether operative or not is to understand the patient’s expectations from their treatment. A mismatch between patient and physician in understanding expectations is bound to end in dissatisfaction for both parties. Adding a statement of expectations to the preoperative consent process is good medicolegal advice.
Putting It Together
The images in Figure 1 demonstrate where many of the above principles are important to consider. These images show the foot of a patient with a painful left 2nd toe. This was an older, community ambulating patient, asking for pain relief. The hallux valgus deformity was painless, and I did not think she could handle reconstructing the first MTP joint to clear space to realign the 2nd toe.
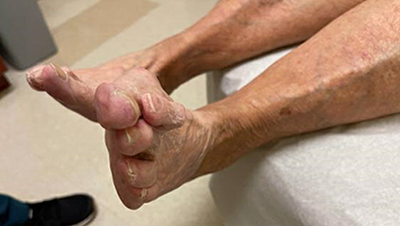
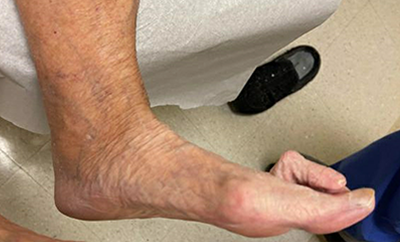
Instead, an option with less surgical intervention and an easier and faster recovery was a simple digital amputation (Figure 2). The patient was immediately weightbearing in a surgical shoe and recovered without complications. Considering what the patient needed rather than embarking on a more complex reconstruction ended with a successful outcome.
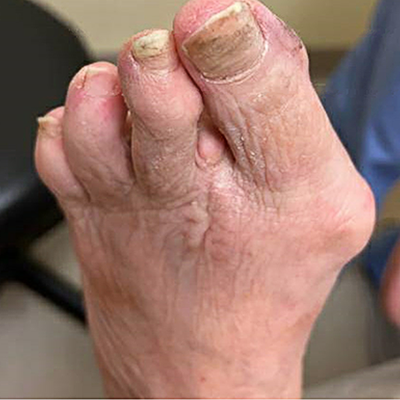
The example demonstrates consideration of several of the components of Rule 4, considering the patient. Age, situational needs, and the ability to bear weight were important considerations, as were tissue quality and expectations. Keeping the needs of the patient in mind while understanding the limitations of her body and what options were available permitted a safe surgical choice that focused on the strained anatomy, recognizing we weren’t going to fix her abnormal biomechanics. A happy patient was the result. Next time we’ll begin delving into the deeper aspects of surgical care with our next rule.
Best wishes.

Jarrod Shapiro, DPM
PRESENT Practice Perfect Editor
[email protected]

































Comments
There are 0 comments for this article