
Practice Perfect 824
Making Practice Perfect Clinical Decisions
Part 1 - Determine the Damaged Anatomy
Making Practice Perfect Clinical Decisions
Part 1 - Determine the Damaged Anatomy

Welcome to the first installment of our ongoing series, Making Practice Perfect Decisions. Today, we’re going to start with the first rule to make treatment decisions.
Now, you may be thinking, “This first rule is so obvious.” Obvious, perhaps, but not always self-evident. When teaching students and residents in the clinic, I will often ask them to tell me what anatomical structure is damaged or strained, and many times they can’t answer. The importance of this first step is to provide an organized approach around which to structure one’s thought process.
For example, consider a 50-year-old female patient complaining of plantar forefoot pain. There are many structures on the plantar foot that can be painful; the trick is figuring out exactly which one. This is accomplished, first, with a detailed history. Through a combination of listening to the patient’s story, asking our own questions, and having a thoroughly complex mental representation (AKA clinical script) of the various possible disorders, we can typically come to a tentative diagnosis before starting the physical examination. This patient with plantar forefoot pain points to the plantar 2nd metatarsal head as the area of maximum pain. It is painful when standing and improves when wearing athletic shoes. She denies digital paresthesias and relates her 2nd toe has started to elevate off the ground. Most of us would think of predislocation syndrome, capsulitis, and a 2nd hammertoe as the most likely diagnoses, leading to the plantar plate as the damaged anatomical structure. On the other hand, if the patient pointed to the plantar 3rd intermetatarsal space and said, “it feels like I’m standing on a rock”, one might think this is a Morton’s neuroma.
Obviously, these are relatively simple disorders, and some are going to be much more complex. For example, lateral ankle instability often involves damaged proprioceptive nerve fibers, ligaments, and sometimes the cartilaginous surfaces of the ankle joint. Similarly, patients with lateral column overload resulting from supinatory deformities such as pes cavus can often be difficult to determine a specific damaged structure for.
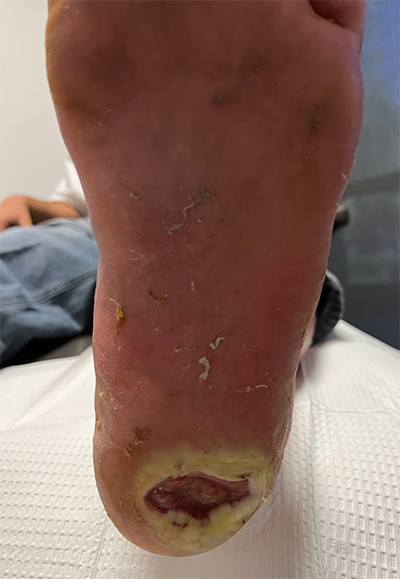
Perhaps the clearest example of determining the damaged or strained anatomy is when diagnosing a neuropathic foot ulcer. Clearly the damaged anatomy is the skin. It is also helpful to understand what aspects of the skin have been damaged. Is it just the epidermis? Does it involve the dermis or subcutaneous layer, or does it also involve the deeper tissues such as bone? Figure 2 shows the unfortunately all too common appearance of a neuropathic heel ulcer with damaged layers of the skin through the subcutaneous layers.
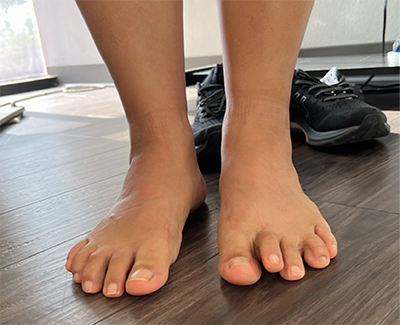
For the lower extremity specialist, the physical examination is almost as important as the history. Our examination methods can often tease out the specifics, determining exactly what anatomical structure is injured. For example, careful palpation of the foot of our 50-year-old patient with presumed predislocation syndrome will differentiate pain at the plantar plate from that associated with the flexor tendon. Perhaps the digital joints themselves are painful. Fine palpation will reveal that the intermetatarsal space is painless, ruling out intermetatarsal bursitis and neuroma. A dorsal drawer test of the 2nd MTP joint with dorsal subluxation and a toe that fails to purchase the ground as in Figure 1 virtually confirms that the plantar plate is damaged.
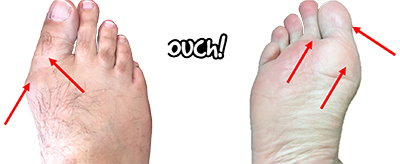
I can’t help but to give one last example. Hallux valgus is very common and mostly an obvious diagnosis. However, a good history and physical examination will, again, tease out the damaged anatomy and yield a more sophisticated understanding of the patient’s deformity. While examining a patient with this diagnosis, palpating the medial first metatarsal head, dorsal joint line, and fibular and tibial sesamoids allows appreciation of the exact nature of the problem and if associated issues such as hallux limitus are also involved. It will also confirm specific aspects of the joint that are damaged (as shown in Figure 3). Similarly, distracting and compressing the joint during range of motion elicits an understanding of synovitis and capsulitis, respectively, as well as an assessment of cartilage integrity.
Although seemingly elementary at first glance, this first principle, determining the specific damaged or strained anatomy, is the first step to yield a full understanding of patients’ diagnoses and guides the rest of the thought process as we’ll see in the future installments of this series.
Best wishes.

Jarrod Shapiro, DPM
PRESENT Practice Perfect Editor
[email protected]

































Comments
There are 0 comments for this article